Diabetic Foot Disease
Foot problems are one of the most common complications of diabetes. They account for more hospital admissions than any other problem in patients with diabetes. The main issues patients with diabetes have with their feet include reduced sensation or alternatively pain (neuropathy) and foot deformity. Diabetics may have poor blood flow to the foot due to atherosclerosis and blocked vessels (peripheral artery disease). They are prone to ulceration and infection including the bone due to reduced immunity and poor wound healing. Diabetes related ulceration and infection is the most common cause of amputation of the leg. Appropriate foot care and wearing appropriate footwear can prevent these complications from occurring.

Patients with diabetes should check their feet daily for dryness, cracking and tinea. Feet should be cleaned, dried and kept well moisturised. Properly fitted comfortable shoes should always be worn including inside the house to protect the feet from injury. Regular podiatry is needed for at-risk patients with diabetes. Callus (a thickened and hardened part of the skin) needs to be debrided (removed) regularly as callus can sometimes hide ulceration which will only be revealed when the callus is removed and without removal of callus infection is more likely.
The development of an ulcer mandates input from several different healthcare professionals. These include your primary care GP, endocrinologist, podiatrist, specialist nurse and a vascular surgeon. All patients with diabetes presenting with a foot ulcer need a full examination of the foot including an assessment of sensation (neuropathy), the circulation (peripheral arterial disease) and the extent of any infection. Understanding the impact of reduced sensation, poor blood flow and infection will dictate the treatment required to heal the ulcer.
The key to management of neuropathic ulcers is relieving the pressure from the area in order to allow it to heal. Pressure relief may be achieved using special footwear or pressure-relieving boots. Some patients may require bed rest potentially in hospital. Regular removal of callus and infected tissue may also be required. Regular appropriate dressings, including those containing antibacterial treatments are also important. Some patients with large ulcers benefit from special suction dressings.
Ulcers related to poor blood flow may be painful and typically require immediate vascular assessment to identify the most appropriate treatment to restore the flow may be achieved either with open surgical bypass or minimally invasive endovascular surgery as with other patients with peripheral arterial disease. Gangrene and amputation are among the most feared complications of diabetes although it usually only occurs when significant peripheral arterial disease is present.
Infection in diabetic foot ulcers can vary from superficial infection to deeper infection of the tissues and bones. Treatment includes antibiotics and in cases of deep infection surgery to remove the infected tissue (debridement). Infection into the bone can be particularly problematic and often requires surgery and prolonged treatment with antibiotics. It is a common reason for toe amputation in patients with diabetes. In patients with diabetic foot infection attention must also be paid to controlling blood sugars and addressing any other medical conditions.
Renal Failure
Patients whose kidneys fail require either renal transplantation, peritoneal dialysis through the abdomen or alternatively haemodialysis where the blood is filtered by a dialysis machine (artificial kidney). Haemodialysis requires large volumes of blood so reliable access to the vascular system is critical. This can be achieved using a plastic tube (catheter) placed into a large vein usually in the neck. However, this is not a permanent solution as they can become infected or blocked and can cause damage to the veins.
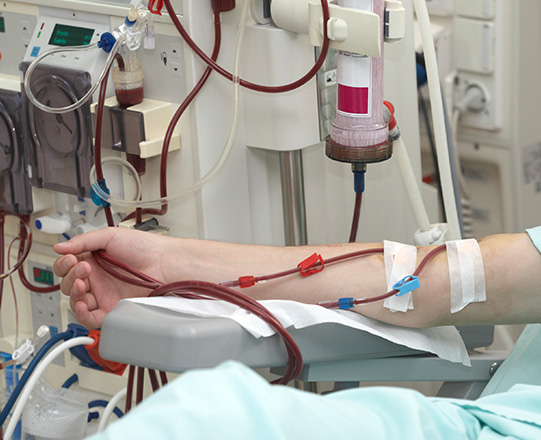
Patients requiring long term haemodialysis are best served with an arteriovenous fistula. These are surgically created by joining an artery to a vein, usually at the wrist or the elbow. After the operation and over a period of 6 to 12 weeks the blood flow through the fistula increases to the point where there is enough flow to support haemodialysis. Once this is the case the fistula can be accessed with needles through the skin and into the vein. Blood is then filtered via a dialysis machine.
Ideally a fistula is created before a patient requires dialysis so that it is ready to use, and a catheter can be avoided. Patients should caution Doctors to avoid placing intravenous lines into the veins at the wrist and elbow to avoid damage to these veins. The non-dominant arm is the preferred location for the fistula to allow greater freedom on dialysis or to facilitate patients dialysing themselves when they are on haemodialysis at home although this cannot always be achieved.
Ideally a patient’s own veins are used to create an arteriovenous fistula. In patients whose veins have been damaged or are not suitable, a synthetic graft can be placed under the skin as an alternative. These grafts have more complications than using a patient’s own veins and typically do not last as long. An ultrasound is used to confirm if a patient’s own veins are suitable and the best area on the arm to create a fistula.
Fistulas can have problems. They may not mature to the point where they can be used therefore some patients may require further procedures. Established fistulas used for dialysis can develop narrowing that may limit blood flow and fistulas may block. Ultrasound surveillance is used to identify issues early so that they can be addressed, and fistula flow maintained. Fistulas can also divert blood flow away for the hand causing pain, if this is the case the fistula may need to be removed in order to restore the circulation to the hand.
Placing the needles into fistulas should be performed by someone appropriately trained (including possibly the patient) under strict hygiene conditions to prevent infection. The buttonhole technique, where the needle is inserted at the same site for each dialysis, is less painful but it can cause local fistula destruction. Area puncture, where the fistula is needled over a specific area, results in the vein expanding over the area and it can also cause narrowing between the expanded areas. The rope-ladder technique, where needles are inserted for each dialysis by moving along the fistula in a sequential pattern, is usually the best technique to prevent fistula destruction.
Hyperhidrosis
Hyperhidrosis is the production of excessive sweat. It can involve the palms of the hands, the arm pits and the feet. This disorder is most intense during adolescence but may abnormally persist into adulthood in some patients. Hyperhidrosis affects approximately 3% of the population. Climate does not cause hyperhidrosis, but hot weather exacerbates sweating. Hyperhidrosis involving the palms and arm pits can be the most debilitating as it often creates substantial professional and social problems for patients.
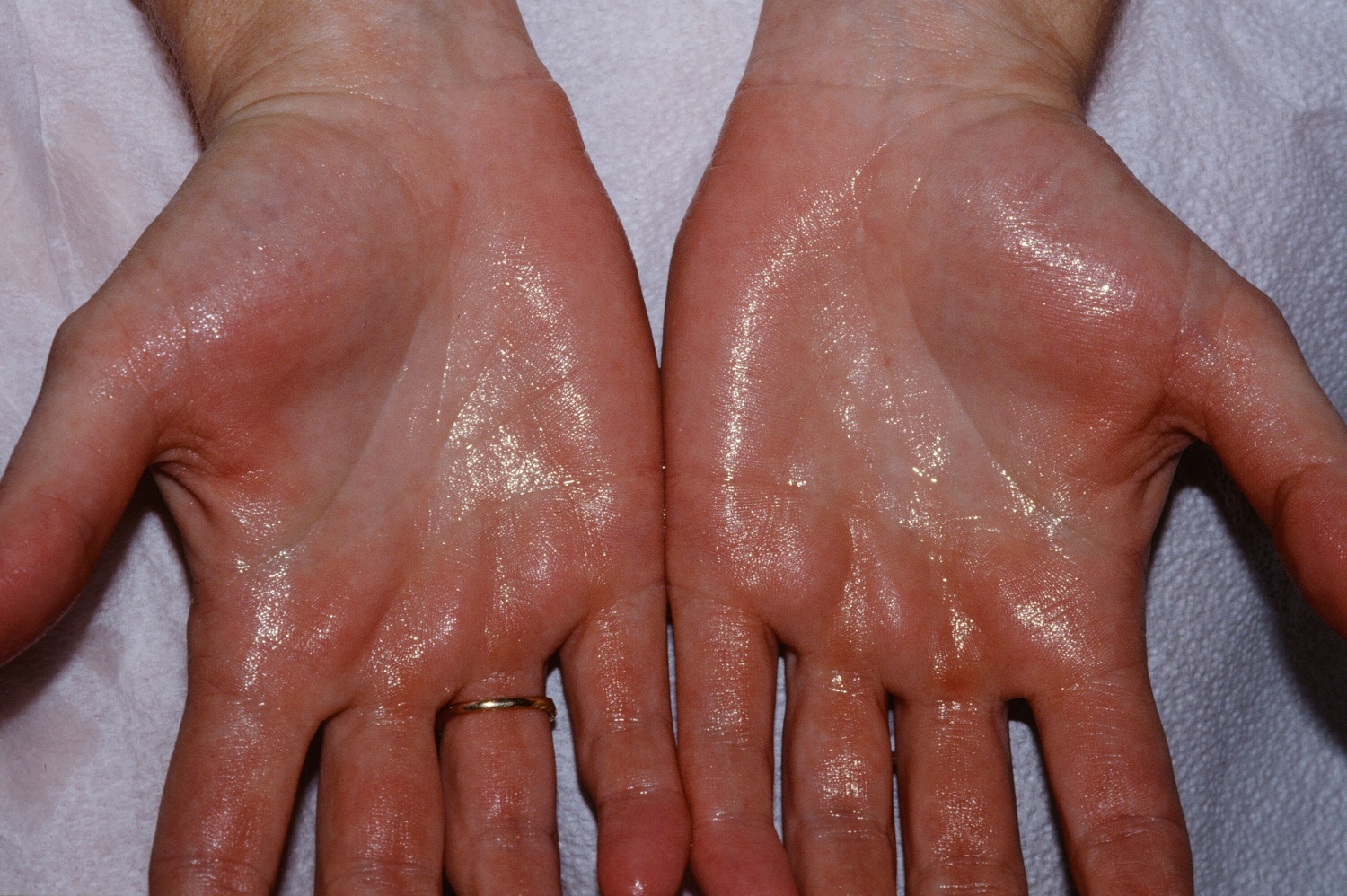
Nonsurgical treatment should initially be attempted in all patients with hyperhidrosis. These include anti-perspirants (especially those containing aluminium chloride), medication (blocks the nerve endings that activate the sweat glands), iontophoresis (the affected areas are placed in water and a low-voltage electrical current passed through it), and Botox injections (directly block the nerves that activate sweat glands). Antiperspirants can cause skin irritation; medication can cause side effects such as a dry mouth and issues passing urine. Iontophoresis and Botox are temporary and need to be repeated regularly which can become expensive.
Surgery to directly cut the nerves in the chest responsible for activation of the sweat glands in the hand and arm pits (thoracoscopic sympathectomy) is an option for patients who do not experience an improvement in quality of life despite appropriate nonoperative treatment. This is a more permanent solution for patients willing to accept the risks involved in surgery. These risks include excess sweating elsewhere (compensatory hyperhidrosis), air in the chest (pneumothorax), bleeding and inadvertent damage to other nerves. Dr Freeman is experienced in performing surgery for hyperhidrosis and can provide expert advice as to whether this is a suitable option for you
Thoracic Outlet Syndrome
Thoracic outlet syndrome occurs when the nerves or vessels (veins and arteries) to the arm are compressed as they come out of the chest, in the space between your collarbone and your first rib ( the thoracic outlet). Dr Freeman is experienced in the management of thoracic outlet syndrome and in performing surgery in appropriately selected patients.
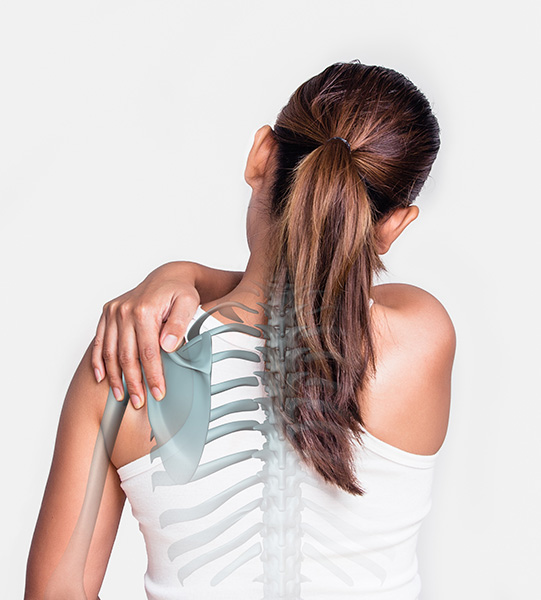
The nerves to the arm may be compressed between the first rib and the clavicle because of a loss of muscle tone, bands crossing the thoracic outlet, abnormalities of the muscles in this area, extra (cervical) ribs, and fracture of the first rib or clavicle. There are particular people who are at risk including for example typists and swimmers. Most patients are in the 25- to 45-year age group and the problem is more common among women than men. The symptoms are pain, pins and needles and weakness in the arm.
Therapy for neurogenic thoracic outlet compression syndrome should always begin with non-operative treatment. This includes exercises and physiotherapy. Patients should avoid heavy lifting and working with the arm above shoulder level. Non-operative treatment should be continued for several months. Many patients will improve significantly and will not require surgery. Indications for surgery include failure of non-operative treatment after several months and persisting disabling symptoms that interfere with work and activities of daily living. The goal of surgery is to create more room for the nerves including possibly removal of any extra (cervical) rib.
The vein taking blood from the arm back to the chest (subclavian vein) can become compressed and develop a blood clot (deep vein thrombosis). This can occur in young patients and is more common in men. Often it occurs during exercise, especially when the arms are above the head. Patients experience pain and swelling in the arm and the arm may turn a bluish colour due to the compression. The main concern here is that there is a risk that a blood clot could travel to the lungs (pulmonary embolus).
Ultrasound will identify most cases of subclavian vein deep vein thrombosis. All patients will need blood thinning treatment. Some patients are suitable for insertion of a tube directly into the vein to deliver medication that will directly dissolve the blood clot. In order to improve blood flow and to create more room for the vein, once the blood clot has been dissolved the first rib may need to be removed. In some cases, the vein may also need to be repaired to prevent further blood clots in the future.
Patients who require a tube (catheter) in the chest veins for medical treatment, for example to administer chemotherapy to treat cancer or for dialysis to treat renal failure, may also develop blood clots in these veins. This is more common with larger catheters like those used for dialysis. Patients may develop swollen arms and the clots can spread to the lungs
(pulmonary embolism). Treatment is with blood thinning medication and the catheter may need to be removed.
Arterial complications are often associated with bony abnormalities including an extra (cervical) rib or fracture of the first rib or clavicle. Compromised circulation to the hand can cause pain, colour changes and pins and needles. In extreme cases, if no treatment is initiated, patients are at risk of gangrene. For this reason patients with arterial thoracic outlet compression syndrome usually requires surgery to create more space for the artery and to and repair the artery in order to restore blood flow to the hand.
