Varicose Veins
Varicose veins are a common problem. They are abnormally prominent veins visible in some people on the thighs and legs. Some patients have fine superficial spider veins. Others have larger varicose veins. Varicose veins can be associated with symptoms such as aching and itchy legs. Some patients will develop swelling, abnormal skin pigmentation or eczema and in advanced cases the skin may break down producing a non-healing wound or ulcer.
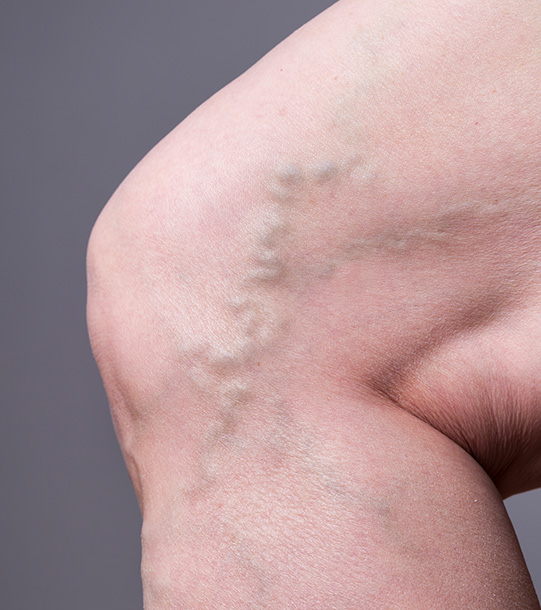
Varicose veins and the associated problems relate to the veins not working properly. Healthy veins normally take blood from the feet back up to the heart. They have valves in them to ensure that the blood only flows in one direction. In some people the valves do not function properly, and the blood refluxes back down the leg. The pressure increases causing the veins to become distended. Fluid can leak out of the veins causing swelling. After a prolonged period of elevated pressures skin changes and ulcers can develop.
Patients have both deep and superficial veins that can have problems. Varicose veins are mostly associated with problems related to the superficial veins. Varicose veins can develop painful blood clots. These are however typically superficial and do not have the same risks associated with deep blood clots (deep vein thrombosis).
If you have concerns about your veins you should get a referral from your General Practitioner (GP) for a vascular assessment. This will include you describing the problems you are having and whether you have had any previous treatments for varicose veins. It is important to disclose if you have a history of blood clots, whether you have any other medical conditions and your current medications, as some medications can cause bleeding or increase the risk of blood clots. Your assessment will also include an examination of your legs including your veins and it would be helpful to dress appropriately for this.
Most patients will need to go on to have an ultrasound scan. This is a non-invasive test used to examine the circulation in the blood vessels of the body and in this case your legs. It is not painful and does not require any injection or radiation. This is usually performed by an experienced vascular sonographer who understands the assessment of patients with venous disease. This test identifies exactly what the problem is, and which veins are involved. Often patients have damaged valves in either the great saphenous vein on the inside of the thigh or leg or the short saphenous vein on the back of the calf.
After your assessment and detailed ultrasound examination advice can be provided in relation to the most suitable treatment. Some patients are best managed with firm compression stockings. Other treatments include injection sclerotherapy, minimally invasive endovenous treatment, gluing of veins or an open surgical procedure known as stripping the veins. Patients with problems related to varicose veins typically can be treated with minimally invasive procedures in order to assist them with their symptoms and the appearance of their legs.
Some patients will get relief from their symptoms and their veins can be controlled by wearing firm compression stockings. Compression stockings promote normal blood flow up the leg. Typically Class II stocking are used, however some patients will only tolerate a less firm Class I stocking. Patients should be specially measured for these stockings. Stockings need to be worn during the day and can be taken off at night. After a period the elastic becomes less effective and new stockings will need to be bought.
Injection sclerotherapy involves injecting the vein with an irritant solution called a sclerosant in order to shrink the vein and shut it down. The body then gets rid of the vein over time. Injection sclerotherapy is performed in the clinic rooms. Sometimes it is done under ultrasound guidance. Patients will need to have compression stocking on their leg for a period after the procedure but can immediately walk, drive and essentially return to normal activity. The risks are soreness and lumps at the injection sites that usually settle over time. Some patients develop skin discolouration and in some cases multiple treatments may be required.
As an alternative to surgical stripping most patients with diseased long or short saphenous veins can be managed these days with a procedure called endovenous treatment. Endovenous treatment uses heat which closes and shrinks the varicose vein causing scar tissue to seal off the vein. A probe is placed into the vein under ultrasound guidance and activated to shut the vein down. The vein is effectively destroyed and as it heals the vein disappears and blood then flows through alternative healthy veins. This has the advantage over surgical stripping of being less invasive. This procedure is less painful than surgery and patients return to normal activity after a shorter period.
A patient’s varicose veins may also need to be directly treated either with surgical removal through a small incision or alternatively injection sclerotherapy performed either at the same time as the endovenous treatment treatment or later.
A more recent treatment for varicose veins that has become available is medical grade glue called VenaSeal™ (cyanoacrylate). This involves the placement of a very small amount of VenaSeal vein glue into the vein through a small catheter. Once the glue enters the vein it seals the affected vein shut, blood is immediately re-routed through other surrounding healthy veins in the leg. This is performed in the clinic rooms under local anaesthetic. Similar to endovenous treatment and injection treatment it is minimally invasive and patients can return to normal activity almost immediately. However not all patients are suitable for this type of procedure. This is dependent on a patient’s ultrasound findings as to whether this is an appropriate treatment. Like endovenous treatment some patients may require additional injection sclerotherapy later.
While open surgery has largely been replaced by minimally invasive procedures, it remains appropriate for selected patients with varicose veins. Surgery involves directly removing diseased veins from the thigh and leg through incisions. Often an incision is placed in the groin where the vein is tied off before being stripped from the leg. Patients can have bleeding, pain related to the incisions and there is a risk of wound infection. Patients normally require a period off work and need to avoid any heavy or strenuous activity.
Varicose veins typically involve the superficial veins. Treating them does not compromise the circulation in the leg. Blood is directed to healthy deep veins and then returned to the heart.
Depending on the severity of the problem patients can be treated in both public and private hospitals. However, most patients are suitable for treatment in the clinic rooms. Patients need to be assessed and have an ultrasound performed by an experienced vascular sonographer to determine the best option.
All treatments do carry with them some risk. In patients with surgical incisions they can have problems with bleeding, wound infection and they will also have small scars that typically fade over time. There is a risk of inflammation after the procedure which settles with anti-inflammatories. Some patients do develop skin discolouration that may not completely fade. Rarely patients develop blood clots which can be prevented with medication. There is also a small risk of nerve damage and associated numbness. Every precaution is taken to avoid these problems. A proportion of patients will need more than one treatment in order to completely manage their veins. Some patients are left with some residual veins.
Prior to pregnancy or between pregnancies patients can have their varicose veins treated. Varicose veins do become worse during pregnancy and this is managed with compression stockings.
Patients who have had previous treatment for veins including surgery in the past may be suitable for further treatment should their varicose veins return.
Some patients have more complex problems related to their veins. These include problems with the pelvic veins and the veins related to the ovaries. In these patients a more comprehensive assessment is required with ultrasound and sometimes computerised tomography (CT). Treatments are individualised for each patient to address these more complex problems. Dr Freeman has extensive experience in the treatment of varicose veins and the treatment of patients with more complex venous problems.
Deep Vein Thrombosis
The most common reason why a patient will suddenly develop a swollen leg is due to the development of a blood clot in the deep veins of the leg (deep vein thrombosis or DVT). The development of DVT is associated with several factors. These include long haul air travel, immobility, surgery, certain medications and several medical conditions. Early diagnosis of the condition is critical in order to prevent the blood clots travelling to the lung and causing damage (pulmonary embolus). A pulmonary embolus is a serious medical emergency with a potentially fatal outcome.
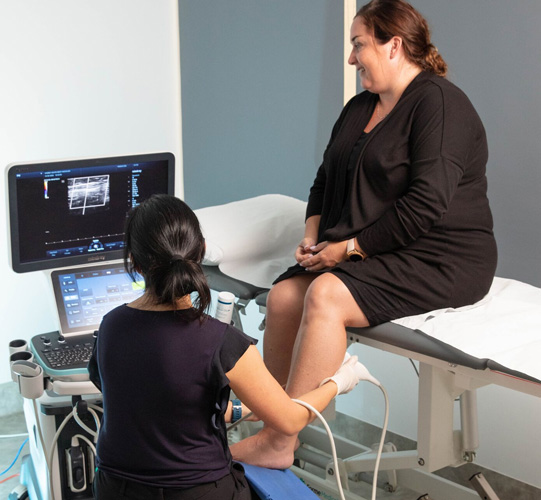
Patients with a swollen leg should seek medical attention as soon as possible and have an ultrasound scan to confirm a DVT. This will show any clots involving the deep veins of the leg (deep vein thrombosis) and appropriate treatment can be started in order to prevent clots spreading to the lungs, a condition known as a pulmonary embolism or a PE. Patients with a swollen leg who are thought to possibly have a DVT can have scans performed in Dr Freeman’s clinic on the same day that they are referred by a GP, and treatment can be started immediately.
These days treatment can either be initially with injections or alternatively blood thinning medications (anticoagulants). Recently tablets have become available that do not require regular blood tests in order to confirm that they are effective in thinning the blood and reducing the risk of the blood clot spreading to the lung. If this is the first diagnosed DVT patients will need to be on the tablets from anywhere between three and twelve months. In some cases patients may require lifelong blood thinning treatment. Patients are strongly advised to also wear compression stockings.
A compression stocking is a device that uses graduated pressure (tighter around the ankle and less pressure as they move up the leg) to help prevent a recurrence of DVT by moving blood through the veins to the heart. Studies show that patients who wear stockings for two years after a significant blood clot are less likely to develop long term complications in the legs such as swelling and skin problems. The stockings need to be specially measured and worn each day in order to prevent the long-term complications related to having deep vein thrombosis. Compression stockings or hosiery is available in several styles and colours, including socks, stockings, knee-highs, and thigh-highs for both men and women, Compression stockings should not be confused with support stockings. Ideally patients should be fitted a Class II stocking if they are able. In addition, patients are encouraged to walk regularly to promote blood flow and assist with helping the clot to dissolve.
In some patients the blood clots will spread to involve the deep veins up in the pelvis or abdomen. This is usually associated with an especially severe swollen leg. Some patients that develop this may be appropriate for a procedure where a catheter is inserted to deliver direct clot-dissolving medication to the deep vein thrombosis (thrombolysis). A mechanical device can also assist in directly removing the clot from the deep veins. These procedures do have some risks, particularly bleeding, and not all patients are suitable for this treatment.
Some patients require insertion of a filter between the blood clot and the lungs in order to stop the blood clot travelling to the lungs. The filter is placed in the vena cava, the main vein in the abdomen. This is especially the case in patients who cannot have blood thinning medication or in whom the blood thinning medication is ineffective. Dr Freeman has had extensive experience in the management of deep vein thrombosis including clot dissolving treatments, patient suitability for a vena cava filter and filter insertion and removal.
Other causes of a swollen leg include problems with the lymphatic system such as lymphoedema, infections in the leg (cellulitis) and ruptured Baker’s cyst (swelling behind the knee). Patients with heart, kidney, liver and thyroid problems can also develop fluid retention and swelling. Usually a careful assessment and appropriate tests can determine the cause of a patient’s swelling.
Leg Ulcers
Ulcers are wounds that are slow to heal or do not heal. They involve loss of skin and tissue on the legs or feet and often relate to vascular problems where the circulation is compromised. The most common cause of leg ulceration relates to venous disease where the veins do not work properly to take blood back up to the heart from the feet. Ulcers can also be caused by blocked arteries (peripheral arterial disease). Patients with diabetes and nerve damage (neuropathy) are also particularly prone to developing ulcers.
Dressings and antibiotics are often not enough to heal ulcers. A thorough assessment of the circulation and treatment to address the underlying cause of the ulcer may assist with healing in patients with both venous and arterial problems. Patients with diabetic nerve damage (neuropathy) also require relief of pressure from the area. Dr Freeman has extensive experience with all these causes of leg and foot ulceration and can provide treatments to assist with ulcer healing.
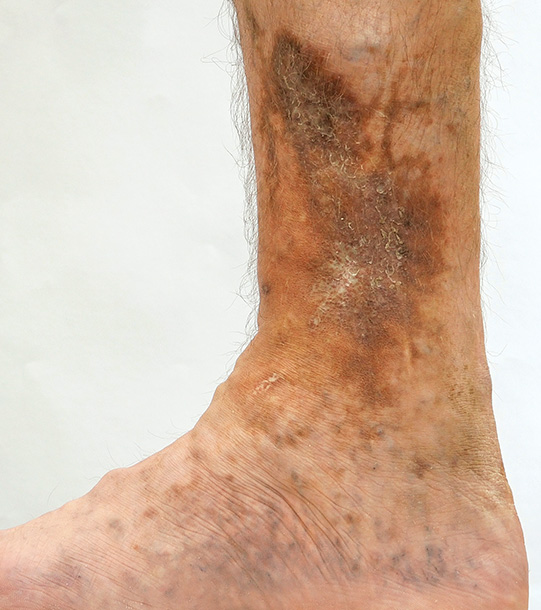
The most common cause of leg ulceration relates to venous disease. This is when the veins do not function properly to take blood from the leg back up to the heart. The pressure rises and fluid leaks out of the veins. This can initially cause swelling. This progresses to causing skin changes such as pigmentation and dermatitis. Finally, the skin can break down causing a wound that does not heal. Venous ulcers may be precipitated by an injury to the leg, including relatively minor trauma. They can be painful and can become infected.
A comprehensive assessment will be performed including a detailed history from the patient regarding their ulcer, this includes any medical problems you have and medications you are on. Patients are assessed with ultrasound studies to examine the circulation and particularly the extent of venous disease involving the superficial and deep veins. The pressures may need be measured in the leg and compared to the arm. These tests are best performed by a specialist vascular sonographer experienced in the assessment of patients with ulcers.
Patients with venous ulcers need regular dressings. If the ulcer is infected, patients will require antibiotic treatment. In addition, following a specialist assessment some patients may be appropriate for formal multi-layer compression bandaging from the toes to the knee. This needs to be applied by an experienced nurse and the bandages left intact until the nurse returns to change and reapply the bandaging. The level of compression is determined by a Specialist and patients need to follow up with the specialist to ensure that the bandages are being appropriately applied.
Compression bandages are usually needed for several weeks. Once the ulcers are healed patients will then be transitioned to wearing a compression stocking in order to prevent the ulcers from returning. It is important that patients are individually measured up for these stockings. Stockings will need to be replaced when the elastic deteriorates, and they become less effective in preventing the ulcers from returning. Stockings need to be worn during the day but can be taken off at night.
Patients with ulcers related to venous disease are encouraged to be active. Regular walking helps promote circulation and can assist with ulcer healing. Some patients may also be suitable for procedures aimed at repairing the diseased veins. These treatments include laser of the refluxing veins or stenting (inserting a small scaffold into) blocked pelvic veins. A proportion of patients might also benefit from open surgery. Dr Freeman can determine which patients are suitable for these treatments and is experienced in performing them.
Pelvic Congestion Syndrome
Some women experience pain and heaviness in the lower abdomen or pelvis related to problems with the veins draining the blood from the pelvis. This is called pelvic congestion syndrome. There are several alternative causes of pelvic pain including problems with the bladder, reproductive organs such as the uterus and ovaries and problems with the gut. Determining which of these causes is most relevant in a woman requires expert assessment and investigation.
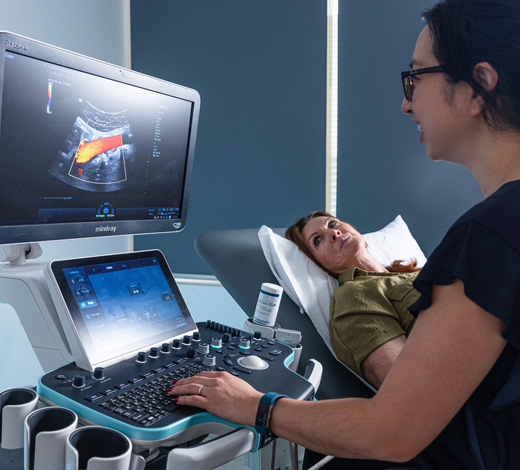
In women with pelvic congestion syndrome the problem can relate to the veins draining blood from the ovaries which is particularly common in the left ovarian veins. Instead of the blood flowing up towards the heart it flows back down into the pelvis and causes the pressure to rise. This is experienced as pain and heaviness in some women. It can be associated with varicose veins deep in the pelvis. However, not all women with varicose veins in their pelvis have pelvic congestion syndrome.
Ultrasound scanning by a specialist vascular sonographer can determine whether a woman has a diseased refluxing ovarian vein causing pelvic varicose veins and potentially pelvic congestion syndrome. Women with pelvic pain and potentially with pelvic congestion syndrome will also need to be assessed by a gynaecologist. They may require other tests such as a pelvic ultrasound, CT scanning and laparoscopy to directly examine the pelvis. Your gynaecologist will advise you in relation to the need for this further testing.
After excluding other causes of pelvic pain Dr Freeman is experienced in treating patients ovarian vein reflux to reduce the pressure in the pelvis. A minimally invasive procedure called coil embolization is used to stop the blood refluxing back down into the pelvis enabling patients to get relief from their pain. Immediately after the procedure the pain may become be worse, this normally settles over a period of days. The procedure is done under local anaesthetic through the groin and patients go home on the same day.
